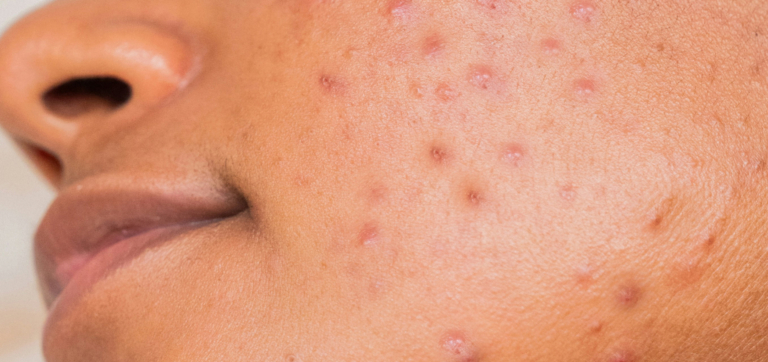
You’ve switched detergents, moisturizers, and diets—more than once. But the itchy flare-ups keep coming. Now, science is turning inward, exploring how the gut—and specific probiotic strains—might influence skin health and offer new support for those with eczema.

Overview
- Eczema, or atopic dermatitis, is a complex inflammatory skin condition where an altered gut microbiome and disrupted gut-skin axis are recognized as contributing factors.
- Specific strains of probiotics—live microorganisms that support health—are being studied for their potential role in skin and immune function in people with eczema-prone skin.
- Not all probiotics work the same way. Each strain has unique properties, and outcomes depend on precise formulation and use.
- Some Lactobacillus and Bifidobacterium strains have shown potential in studies, though results can vary and research is still unfolding.
- Important considerations include strain specificity, dosage, delivery, and product quality.
- Talk to a healthcare provider before starting a new product, especially for children, infants, or during pregnancy.
It starts with the itch. Then the flare-up. Then the second-guessing—Was it something you ate? The weather? Your laundry detergent again?
Eczema (also known as atopic dermatitis or AD) isn’t just about dry skin. It’s itchy, inflamed, scaly, and often frustratingly unpredictable. And after you’ve tried every steroid cream and swapped out every ingredient in your routine, it’s only natural to start looking deeper—like inside your gut, where probiotics for eczema are being studied for how they might support skin health from the inside out.
Researchers are now looking into how gut microbes may influence immune responses and barrier function—two major players in eczema. It’s a shift that’s opening up new questions about how microbial balance inside the body might shape what shows up on the skin.
Even though it may seem like it, eczema doesn’t just show up—it builds on layers of immune overreactions, a weakened skin barrier, and triggers that don’t always make sense. (🧴 Insert sad shelf of rejected moisturizers and trigger suspects here.)
Understanding those layers is the first step toward figuring out what might actually help.
Understanding Eczema: More Than Just Skin Deep
Eczema is one of the most common inflammatory skin conditions, affecting adults and children. It often presents as dry, itchy, inflamed skin—but the toll isn’t just physical. It can disrupt sleep, increase stress, and affect quality of life.1
While no single cause explains eczema, several contributing factors include:
- Genetics: A family history of eczema, asthma, or hay fever may raise the risk.2
- Immune Dysregulation: Eczema typically involves an exaggerated immune reaction to everyday triggers.3
- Barrier Impairment: The skin’s protective layer may be less effective in those with eczema, allowing moisture loss and irritant entry.4,5
- Environmental Triggers: These include harsh soaps, seasonal changes, allergens, and stress.6
- The Microbiome: Researchers are examining how changes in the gut microbiome and the skin microbiome may influence eczema symptoms.7
The Gut-Skin Axis: How Your Gut Talks to Your Skin
The gut-skin axis refers to the two-way communication between your gut and skin. It involves the gut microbiome, immune system, and signaling molecules.8
Your gut hosts trillions of microbes that help:
- Break down food and absorb nutrients 9
- Produce certain vitamins
- Regulate immune responses
- Maintain the gut barrier (which controls what gets into your bloodstream)8
When your gut microbiome is healthy and balanced, it keeps things running smoothly—inside and out. But when that balance is thrown off (a state called dysbiosis), it may loosen the gut barrier, sometimes referred to as “leaky gut.”10 That means substances like bacterial byproducts or bits of undigested food can slip into the bloodstream, where they might stir up inflammation that shows up on your skin—especially in conditions like eczema.8
Probiotics and Eczema: What Does the Research Show?
Not all probiotics have the same effects. The potential effect of a probiotic depends on the specific strain, the amount used, and whether it’s been studied for a targeted purpose, like immune regulation or gut barrier support. When you’re dealing with something as complex as eczema, precision matters.
This reflects the scientific consensus that probiotic effects are both strain-specific and dose-dependent.11
How Probiotics May Support Eczema-Prone Skin
Researchers have found several potential mechanisms of action used by probiotics in this context:8
- Immune Modulation: Some strains may help balance immune responses, potentially through effects on T cells involved in inflammation.
- Gut Barrier Support: Certain probiotics may support the gut lining, making it less permeable to inflammatory triggers.
- Microbial Balance: Probiotics can compete with unwanted microbes, helping to maintain a more balanced internal environment.
- SCFA Production: Some strains produce short-chain fatty acids (like butyrate), which nourish gut lining cells and may have anti-inflammatory effects.8
What Probiotic Strains Help With Eczema?
Research on probiotics and eczema focuses on individual strains, not broad categories. Here’s what some of the science shows:
- L. rhamnosus GG: One of the most studied strains for eczema—especially for prevention in infants when taken during pregnancy or early infancy. Some studies suggest it may reduce eczema severity, though findings vary.12,13
- L. salivarius LS1: Studied for its role in reducing gut permeability and easing symptoms in adults with eczema.14
- B. breve BR3: Explored for immune-modulating properties and symptom improvement in adults.15
- B. lactis CECT8145: Studied in dermatology-focused probiotic blends for its potential to support skin function and microbiome balance.
- B. lactis (various strains): Some strains have shown potential to support skin health, particularly in children.16 (Yes, probiotics for kids are a real thing!)
- B. longum CECT7347 and L. casei CECT9104: Also included in probiotic formulations studied for dermatological support.17
When researchers review multiple studies together, the results tend to vary. That doesn’t mean probiotics aren’t helpful, but it does show how much the details matter: the exact strain used, the dosage, the population studied (like children vs. adults), and how long the probiotic is taken.
These differences significantly affect outcomes, which is why strain-specific, well-designed studies are extremely important when considering probiotics for eczema. (Check the probiotics bottle and their website!)
Beyond Probiotic Strains: What Else Matters?
Even the right strain won’t do much without the right delivery and formulation.
- Dosage: Probiotics are measured in CFU (colony-forming units) or AFU (active fluorescent units). CFU counts only the microbes growing on a petri dish, but AFU uses advanced technology to count all viable, active cells—including those that are alive but not culturable. This makes AFU a more precise way to count the actual number of microbes capable of doing their job in the body.
- Delivery Technology: Probiotics need protection from stomach acid to reach the gut alive. Capsule designs vary in effectiveness.
- Synbiotics: These pair probiotics (beneficial microbes) with prebiotics (the nutrients they eat.) Together, they can support the survival and activity of your gut microbes. Some formulations include polyphenol-rich ingredients (like Indian pomegranate) that microbes turn into compounds—like urolithin A, which is being studied for its potential effects on inflammation and cellular function.18,19
- Consistency: Because the beneficial microbes don’t stick around after stopping probiotics, their benefits are linked to ongoing daily use.20
Dietary and Lifestyle Approaches for Eczema-Prone Skin
Probiotics are only one piece of the puzzle. A well-rounded approach for managing eczema-prone skin includes:
- Diet: Some people react to certain foods. Avoiding triggers and focusing on whole, nutrient-rich meals may support the skin and gut.21
- Skincare: Stick with gentle cleansers, moisturizers that support barrier function, and products with a skin-friendly pH.22
- Stress Management: Chronic stress may influence eczema flares.8 Practices like meditation, exercise, or therapy can help.
- Hydration: Adequate water intake helps support skin resilience.23
Probiotics shouldn’t replace medical treatment. If you’re considering a probiotic for eczema, talk with your healthcare provider—especially for children, during pregnancy, or when managing other conditions.24
The Key Insight
Living with eczema means living with unpredictability—itchy flare-ups that come out of nowhere, scaly patches that seem to resist every kind of cream, and the red, inflamed skin that can make even showers feel painful. It’s rarely just “dry skin.” It’s a long-term, whole-body condition with roots in immune imbalance, barrier dysfunction, and—as recent research shows—microbial shifts in the gut. (This is why the gut-skin axis matters!)
Probiotics aren’t a cure, but some strains have been studied for their potential to support gut barrier integrity and immune responses that affect the skin. Not all strains are created equal, and not all products deliver them effectively—but the science is beginning to uncover which ones matter, how they work in the body, and what it takes to get results.
🌱 Because for something as persistent and personal as eczema, it’s not about adding bacteria—it’s about med-locking your system with purpose.
Frequently Asked Questions (FAQs)
Can Probiotics Make Eczema Worse?
Probably not. For most people, probiotics are generally safe and well-tolerated. Some people might notice temporary digestive changes when they start probiotics—like mild gas or bloating—as the gut microbiome adjusts.
If symptoms persist or your eczema worsens, stop taking the product and consult your healthcare provider. Look for products with specific, studied strains to reduce the chance of unwanted reactions.
Which Probiotic Strain Is Best For Skin Or Eczema?
There’s no single “best” strain for everyone. But some strains from the Lactobacillus genus (like L. rhamnosus GG and L. salivarius) and Bifidobacterium group (such as B. lactis and B. breve) have been studied for their potential to support skin health and help balance immune responses in people with eczema.
Formulations including L. salivarius LS1 or B. breve BR3 are examples that have been researched for skin health support. 💡Pro tip: make sure the strains are listed clearly and backed by clinical studies.
How Long Does It Take For Probiotics To Show An Effect On Eczema-Prone Skin?
It depends. Some studies suggest changes may occur within a few weeks, while others show it may take several months of consistent daily use. Results vary based on the strain, the person’s microbiome, severity of eczema, and other lifestyle factors.
Probiotics don’t work instantly—they need time to interact with your system.
Should I Focus On Probiotics Or Prebiotics For Eczema Support?
Both can help. Probiotics introduce beneficial microbes, while prebiotics feed the microbes already in your gut (or the ones in your probiotic). A synbiotic—combining both—can offer more comprehensive support.
Some prebiotics, like those derived from Indian pomegranate, are being studied for their ability to support the production of compounds like urolithin A, which may influence inflammation and cellular processes.
Citations
- Chovatiya, R. (2023). Atopic Dermatitis (Eczema). JAMA, 329(3):268. https://doi.org/10.1001/jama.2022.21457
- Ferreira, M. A., Vonk, J. M., Baurecht, H., Marenholz, I., Tian, C., Hoffman, J. D., Helmer, Q., Tillander, A., Ullemar, V., van Dongen, J., Lu, Y., Rüschendorf, F., Esparza-Gordillo, J., Medway, C. W., Mountjoy, E., Burrows, K., Hummel, O., Grosche, S., Brumpton, B. M., Witte, J. S. (2017). Shared genetic origin of asthma, hay fever and eczema elucidates allergic disease biology. Nature Genetics, 49(12):1752-57. https://doi.org/10.1038/ng.3985
- Bauer, S. M. (2017). Atopic Eczema: Genetic Associations and Potential Links to Developmental Exposures. International Journal of Toxicology, 36(3):187-98.
- Proksch, E., Fölster-Holst, R., Jensen, J. M. (2006). Skin barrier function, epidermal proliferation and differentiation in eczema. Journal of Dermatological Science, 43(3):159-69. https://doi.org/10.1016/j.jdermsci.2006.06.003
- Wang, X., Ye, L., Lai, Q., Wen, S., Long, Z., Qiu, X., Elias, Peter M., Yang, B., Man, M.Q. (2020). Altered Epidermal Permeability Barrier Function in the Uninvolved Skin Supports a Role of Epidermal Dysfunction in the Pathogenesis of Occupational Hand Eczema. Skin Pharmacology and Physiology, 33(2):94-101. https://doi.org/10.1159/000506425
- Tamagawa-Mineoka, R. & Katoh, N. (2020). Atopic Dermatitis: Identification and Management of Complicating Factors. International Journal of Molecular Sciences, 21(8):2671. https://doi.org/10.3390/ijms21082671
- Lee, S. Y., Lee, E., Park, Y. M., Hong, S. J. (2018). Microbiome in the Gut-Skin Axis in Atopic Dermatitis. Allergy, Asthma & Immunology Research, 10(4):354-62. https://doi.org/10.4168/aair.2018.10.4.354
- Salem, I., Ramser, A., Isham, N., Ghannoum, M. A. (2018). The Gut Microbiome as a Major Regulator of the Gut-Skin Axis. Frontiers in Microbiology, 9:1459. https://doi.org/10.3389/fmicb.2018.01459
- Krajmalnik‐Brown, R., Zehra‐Esra, I., Kang, D., DiBaise, J. K. (2012). Effects of Gut Microbes on Nutrient Absorption and Energy Regulation. Nutrition in Clinical Practice, 27(2):201-14. https://doi.org/10.1177/0884533611436116
- Dmytriv, T. R., Storey, K. B., Lushchak, V. I. (2024). Intestinal barrier permeability: the influence of gut microbiota, nutrition, and exercise. Frontiers in Physiology, 15. https://doi.org/10.3389/fphys.2024.1380713
- Hill, C., Guarner, F., Reid, G., Gibson, G. R., Merenstein, D. J., Pot, B., Morelli, L., Canani, R. B., Flint, H. J., Salminen, S., Calder, P. C., Sanders, M. E. (2014). Expert consensus document. The International Scientific Association for Probiotics and Prebiotics consensus statement on the scope and appropriate use of the term probiotic. Nature Reviews Gastroenterology & Hepatology, 11(8):506-14. https://doi.org/10.1038/nrgastro.2014.66
- Kalliomaki, M., Salminen, S., Arvilommi, H., Kero, P., Koskinen, P., Isolauri, E. (2001). Probiotics in primary prevention of atopic disease: a randomised placebo-controlled trial. The Lancet, 357(9262):1076-79. https://doi.org/10.1016/s0140-6736(00)04259-8
- Szajewska, H. & Horvath, A. (2018). Lactobacillus rhamnosus GG in the Primary Prevention of Eczema in Children: A Systematic Review and Meta-Analysis. Nutrients, 10(9):1319. https://doi.org/10.3390/nu10091319
- Drago, L., De Vecchi, E., Toscano, M., Vassena, C., Altomare, G., Pigatto, P. (2014). Treatment of Atopic Dermatitis Eczema With a High Concentration of Lactobacillus salivarius LS01 Associated With an Innovative Gelling Complex. Journal of Clinical Gastroenterology, 48(Suppl.1):S47-51. https://doi.org/10.1097/mcg.0000000000000249
- Iemoli, E., Trabattoni, D., Parisotto, S., Borgonovo, L., Toscano, M., Rizzardini, G., Clerici, M., Ricci, E., Fusi, A., Vecchi, E. D., Piconi, S., Drago, L. (2012). Probiotics Reduce Gut Microbial Translocation and Improve Adult Atopic Dermatitis. Journal of Clinical Gastroenterology, 46:S33-40. https://doi.org/10.1097/mcg.0b013e31826a8468
- Kim, J. Y., Kwon, J. H., Ahn, S. H., Lee, S. I., Han, Y. S., Choi, Y. O., Lee, S. Y., Ahn, K. M., Ji, G. E. (2009). Effect of probiotic mix (Bifidobacterium bifidum, Bifidobacterium lactis, Lactobacillus acidophilus) in the primary prevention of eczema: a double‐blind, randomized, placebo‐controlled trial. Pediatric Allergy and Immunology, 21(2p2):e386-93. https://doi.org/10.1111/j.1399-3038.2009.00958.x
- Navarro-López, V., Ramírez-Boscá, A., Ramón-Vidal, D., Ruzafa-Costas, B., Genovés-Martínez, S., Chenoll-Cuadros, E. Carrión-Gutiérrez, M., de la Parte, J. H., Prieto-Merino, D., Codoñer-Cortés, F. M. (2017). Effect of Oral Administration of a Mixture of Probiotic Strains on SCORAD Index and Use of Topical Steroids in Young Patients With Moderate Atopic Dermatitis. JAMA Dermatology, 154(1):37. https://doi.org/10.1001/jamadermatol.2017.3647
- D’Amico, D., Andreux, P. A., Valdés, P., Singh, A., Rinsch, C., Auwerx, J. (2021). Impact of the Natural Compound Urolithin A on Health, Disease, and Aging. Trends in Molecular Medicine, 27(7):687-99. https://doi.org/10.1016/j.molmed.2021.04.009
- D’Amico, D., Fouassier, A. M., Faitg, J., Hennighausen, N., Brandt, M., Konstantopoulos, D., Rinsch, C., Singh, A. (2023). Topical application of Urolithin A slows intrinsic skin aging and protects from UVB-mediated photodamage: Findings from Randomized Clinical Trials. MedRxiv (Cold Spring Harbor Laboratory). https://doi.org/10.1101/2023.06.16.23291378
- Ciorba, M. A. (2012). A Gastroenterologist’s Guide to Probiotics. Clinical Gastroenterology and Hepatology, 10(9):960-68. https://doi.org/10.1016/j.cgh.2012.03.024
- Wollenberg, A., Christen‐Zäch, S., Taieb, A., Paul, C., Thyssen, J. P., de Bruin‐Weller, M., Vestergaard, C., Seneschal, J., Werfel, T., Cork, M. J., Kunz, B., Fölster‐Holst, R., Trzeciak, M., Darsow, U., Szalai, Z., Deleuran, M., von Kobyletzki, L., Barbarot, S., Heratizadeh, A., Gieler, U. (2020). ETFAD/EADV Eczema task force 2020 position paper on diagnosis and treatment of atopic dermatitis in adults and children. Journal of the European Academy of Dermatology and Venereology, 34(12):2717-44. https://doi.org/10.1111/jdv.16892
- Ito, T. & Nakamura, Y. (2024). The skin barrier and microbiome in infantile atopic dermatitis development: can skincare prevent onset? International Immunology, 36(11):579-84. https://doi.org/10.1093/intimm/dxae038
- Dmitrieva, N. I., Boehm, M., Yancey, P. H., Enhörning, S. (2024). Long-term health outcomes associated with hydration status. Nature Reviews Nephrology, 20(5):275-94. https://doi.org/10.1038/s41581-024-00817-1
- Doron, S. & Snydman, D. R. (2015). Risk and safety of probiotics. Clinical Infectious Diseases, 60(Suppl.2):S129-34. https://doi.org/10.1093/cid/civ085