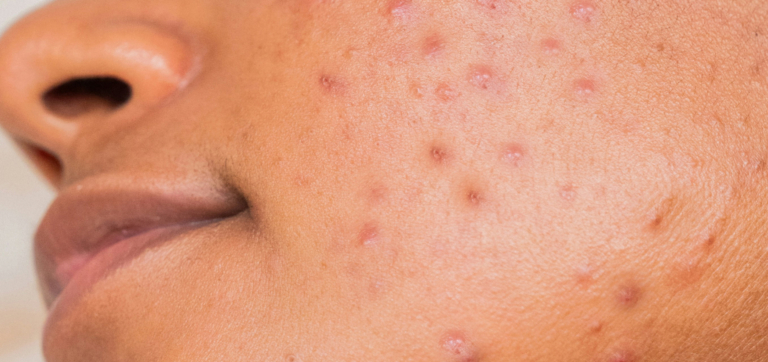
Rosacea doesn’t always respond to creams or careful skincare routines. Some scientists are looking deeper—into the gut—to understand how probiotics might help support skin that stays calmer, longer.

Overview
- Rosacea is an inflammatory skin condition with complex causes and highly personal triggers.
- The gut-skin axis links your digestive health to what shows up on your skin—including redness, bumps, and flare-ups.
- Some probiotic strains may support gut barrier integrity and regulate immune responses that contribute to skin inflammation.
- Early research connects gut imbalances with rosacea, but studies on specific probiotics that can help are limited.
- Probiotics for rosacea aren’t a cure—but the right ones might be a supportive addition to your overall skincare plan.
You’ve tried switching skincare products and cutting triggers out of your diet (including your favorite snack! 🙁) You’ve even iced your face after a flare-up. And still, the redness and bumps just keep coming back—without warning, without reason. Rosacea is unpredictable, and for many people, the usual fixes just don’t cut it. That’s why some researchers are turning inward—literally—to the gut.
Emerging science around the gut-skin axis suggests your digestive system might be doing more than just breaking down food—it could also be shaping how your skin responds to inflammation.
That’s where probiotics for rosacea enter the conversation. Not as a cure, but as a potential way to support skin health from the inside out.
Understanding Rosacea: More Than Just a Blush
Rosacea isn’t just about blushing easily or turning red during stressful moments. If you’re dealing with it, you know it’s an ongoing challenge marked by facial redness, persistent flushing, visible blood vessels, and sometimes acne-like bumps or thickened skin.1 Beyond physical discomfort, rosacea can also feel frustratingly unpredictable, disrupting daily life and social confidence.
The exact cause of rosacea is still unclear. However, researchers agree that it’s an inflammatory condition that can be influenced by several factors.
Some causes include:
- Genetics
- Environmental triggers
- Immune responses
- Neurovascular factors
Common rosacea triggers can include:
- Sun exposure
- Emotional stress
- Spicy foods
- Alcohol
- Hot beverages
- Certain skincare products
Because triggers vary widely between individuals, managing rosacea often feels less like following a clear roadmap and more like solving a personal puzzle—one that standard treatments don’t always fully resolve. It’s this frustration that often leads people to look beyond conventional care, exploring supportive approaches that might address underlying factors like inflammation.1
The Gut-Skin Axis: Could Your Gut Be Fueling Your Flare-Ups?
You may not realize it, but your gut and your skin are always chit-chatting. This constant conversation, known as the gut-skin axis, links your digestive health directly to skin health through immune responses, nervous system signals, and inflammatory pathways.2
Here’s the gist: your gut is home to trillions of microorganisms—bacteria, viruses, fungi, and archaea—collectively known as the gut microbiota. A balanced and diverse gut microbiota is vital for digestion, nutrient absorption, immune system health, and even mood regulation. When this delicate ecosystem gets disrupted—a state called dysbiosis—it can increase gut permeability (often called “leaky gut”) and trigger systemic inflammation.3
Research shows that gut dysbiosis and a weakened gut barrier may allow inflammatory substances and microbial byproducts to enter your bloodstream. This can amplify inflammation elsewhere in the body, including your skin—potentially worsening conditions like rosacea or eczema, which are driven by inflammation.4
Probiotics for Rosacea: How They May Help
Now, let’s talk probiotics. These are live, friendly microbes that can give your gut a boost when taken in the right amounts.5 The idea is pretty straightforward: by helping your gut stay balanced, probiotics might indirectly calm inflammation and support healthier skin, which could be especially helpful for people dealing with rosacea.
Here’s what probiotics might be able to do for your rosacea-prone skin:
1. Calming Inflammation
Some probiotic strains can have conversations with your immune system, helping it stay calm and balanced instead of overreacting.3 Considering rosacea is driven by inflammation, this makes probiotics pretty interesting allies.
2. Strengthening Your Gut Barrier
A sturdy gut barrier helps keep the wrong things out of your bloodstream. Certain probiotics are being studied because they might help strengthen this barrier, keeping inflammatory triggers where they belong—out of circulation.
3. Supporting Your Immune System
Your gut is a major immune-system headquarters. Probiotics might help maintain good immune communication and responses, potentially keeping your body’s defenses running smoothly.6
☝️ Important Note:
While all of these probiotic mechanisms sound promising, research that specifically targets rosacea is still in progress. So, probiotics could be helpful, but it’s important to keep expectations realistic.
Research on Probiotics for Rosacea (So Far)
Here’s where we’re at: early research is hopeful, showing probiotics might help ease skin inflammation, strengthen the skin barrier, and reduce sensitivity.7
We also know that people with rosacea often have noticeable differences in their gut microbiome compared to those without the condition. That imbalance may fuel inflammation, making probiotics a promising candidate for restoring gut balance.
But let’s be clear—more extensive studies are needed to truly understand and confirm these potential benefits.8
Oral vs. Topical Probiotics—What’s the Difference?
When considering probiotics for rosacea, you’ve got two main players: oral (taken by mouth, usually as one or two capsules per day) and topical (applied directly to your skin).
💊 Oral probiotics target the gut-skin axis, working from the inside out by balancing your gut microbiome to potentially support healthier skin. Because the gut microbiome influences multiple systems in the body, these probiotics may also support digestive function, immune regulation, and even mood—benefits that extend well beyond the surface.
🧴 Topical probiotics work from the outside in, applying beneficial bacteria directly onto your skin to balance its microbiome right where symptoms are most visible.9
How to Choose and Use Probiotics for Rosacea-Prone Skin
Not all probiotics are created equal. If you’re considering one for rosacea-prone skin, here’s what matters:
Clinically Studied Strains
Not all probiotics play the same position on the field—even when they’re from the same species. That’s because probiotic benefits are strain-specific—meaning only certain strains have been studied and shown to support specific outcomes.10
When it comes to probiotics, generic labels like Lactobacillus or Bifidobacterium don’t tell you much. What really counts is the strain ID—that string of letters and numbers that follows the species name. That’s where the science lives. For example, L. salivarius LS1 and B. breve BR3 have been studied for their potential effects on skin barrier function. But heads up: that doesn’t mean they’ve been tested for rosacea specifically.11
💡 Pro Tip: If a product doesn’t list full strain names, it’s impossible to know what you’re actually getting—or if it’s been clinically studied for what you care about.
AFU or CFU Counts
Those ginormous numbers on probiotic bottles—like “10 billion CFU”—sound impressive, but here’s the catch: not all those microbes are necessarily alive or active when you take them.
CFU (Colony Forming Units) is the traditional way of measuring probiotics, only counting microbes that can grow on a petri dish. AFU (Active Fluorescent Units), on the other hand, uses a more advanced method—flow cytometry—to count all viable cells, even ones that are alive but not necessarily culturable.
🦠 Why It Matters: AFU gives a clearer picture of how many living microbes are actually capable of doing something in your body. And whichever method a brand uses, look for a guarantee of that count through the product’s expiration date, not just at the time of manufacturing.
Delivery Matters: Survival Isn’t Guaranteed
Your stomach is great at breaking things down—and probiotics are no exception. For those beneficial bacteria to have a chance at doing their job, they need to survive the acidic pit stop and actually make it to your colon alive.
That’s where delivery design comes in. Some products use advanced technologies (like capsule-in-capsule systems) to protect probiotics during digestion and time their release further down in your gut. In other words, without a protective delivery system, those friendly microbes might never make it to where they’re needed.
Realistic Expectations: What You Might Notice—and When
You may not see skin changes right away. Probiotics work indirectly by supporting gut health, and those effects take time.
Some people notice improved digestion or reduced bloating within a few weeks. If probiotics are going to affect your skin, it’s usually further downstream—often after several months of consistent use. And yes, there may be an initial adjustment period with mild bloating or gas.
Go slow. Stay consistent. Be patient. Probiotics aren’t quick fixes—but they’re in it for the long game.
A Whole-Body Approach: Probiotics Aren’t the Only Tool
Probiotics can support skin health—but they work best as part of a broader routine.
For rosacea, a combination of strategies often leads to better results:
- Diet: Certain foods can trigger flare-ups. Common offenders? Alcohol, spicy dishes, and hot beverages. Try keeping a food journal to spot your personal patterns.7
- Lifestyle: Chronic stress and sun exposure can be two major triggers for rosacea.12 That means sunscreen and stress-reduction techniques might be your new BFFS.
- Skincare: Look for fragrance-free, alcohol-free products and avoid anything that vigorously exfoliates or stings.13 Your skin barrier will thank you. 🙏
- Dermatology Support: A board-certified dermatologist can help you navigate flare-ups and tailor a plan that might include topicals, oral medications, or other therapies.
Remember: Probiotics can support this kind of approach—but think of them as part of the team, not the entire playbook.
The Key Insight
The gut-skin axis offers a science-backed way to understand how your gut health can influence what shows up on your skin. For rosacea—where inflammation and immune overreactions drive much of the story—that connection is worth paying attention to.
Probiotics aren’t a cure for rosacea, but some strains have been studied for their potential to support gut barrier function and help calm inflammatory signaling. If the product is strain-specific, clinically studied, and taken consistently over time, that might lead to visible changes on your skin—the kind that won’t make you want to cancel plans.
Because when you’re managing something as stubborn and skin-deep as rosacea, the real story might be happening deeper down. It’s not just about what you apply on the surface, but also the signals coming from within—and whether your microbes are helping calm the noise or adding to it.
🌱 Sometimes, the clearest path to healthier skin doesn’t start in the mirror—it starts in your microbiome.
Frequently Asked Questions (FAQs)
Can Probiotics Make Rosacea Worse?
Not usually. Most well-studied probiotics are safe and well-tolerated. Some people may experience mild digestive symptoms like gas or changes in poop habits during the first few weeks—this is part of the normal adjustment process. If symptoms persist or skin reactions worsen, check in with your doctor.5
What Is the Best Probiotic Strain for Rosacea?
There’s no single “best” strain confirmed for rosacea. But certain strains of Lactobacillus and Bifidobacterium have been studied for their ability to support gut barrier function and modulate inflammation—two factors linked to rosacea symptoms.7
When shopping for probiotics for rosacea, the focus should be on choosing a high-quality product with clinically studied strains known for overall gut health and immune support.
How Long Does It Take for Probiotics to Help Rosacea?
It depends. Digestive changes—like improved regularity or less bloating—may show up within a few weeks. Any skin-related benefits are typically indirect and can take months, as they rely on longer-term changes in gut and immune health.6
Are Oral or Topical Probiotics Better for Rosacea?
Oral probiotics are better supported by science right now. They act systemically (whole-body) by supporting the gut-skin axis.2 Topical probiotics may one day play a role, but for rosacea, the evidence is still early-stage.9
Citations
- Sharma, A., Kroumpouzos, G., Kassir, M., Galadari, H., Goren, A., Grabbe, S., & Goldust, M. (2022). Rosacea management: A comprehensive review. Journal of cosmetic dermatology, 21(5), 1895–1904. https://doi.org/10.1111/jocd.14816
- Salem, I., Ramser, A., Isham, N., & Ghannoum, M. A. (2018). The gut microbiome as a major regulator of the gut-skin axis. Frontiers in Microbiology, 9, 1459. https://doi.org/10.3389/fmicb.2018.01459
- Yoo, J., Groer, M., Dutra, S., Sarkar, A., & McSkimming, D. (2020). Gut Microbiota and Immune System Interactions. Microorganisms, 8(10), 1587–1587. https://doi.org/10.3390/microorganisms8101587
- De Pessemier, B., Grine, L., Debaere, M., Maes, A., Paetzold, B., & Callewaert, C. (2021). Gut–skin axis: Current knowledge of the interrelationship between microbial dysbiosis and skin conditions. Microorganisms, 9(2), 353. https://doi.org/10.3390/microorganisms9020353
- Hill, C., Guarner, F., Reid, G., Gibson, G. R., Merenstein, D. J., Pot, B., Sanders, M. E. (2014). The International Scientific Association for Probiotics and Prebiotics consensus statement on the scope and appropriate use of the term probiotic. Nature Reviews Gastroenterology & Hepatology, 11(8):506-14. https://doi.org/10.1038/nrgastro.2014.66
- Zheng, Y., Zhang, Z., Tang, P., Wu, Y., Zhang, A., Li, D., Wang, C. Z., Wan, J. Y., Yao, H., Yuan, C. S. (2023). Probiotics fortify intestinal barrier function: a systematic review and meta-analysis of randomized trials. Frontiers in Immunology, 14:1143548. https://doi.org/10.3389/fimmu.2023.1143548
- Manfredini, M., Barbieri, M., Milandri, M., & Longo, C. (2025). Probiotics and Diet in Rosacea: Current Evidence and Future Perspectives. Biomolecules, 15(3), 411. https://doi.org/10.3390/biom15030411
- Daou, H., Paradiso, M., Hennessy, K., & Seminario-Vidal, L. (2021). Rosacea and the Microbiome: A Systematic Review. Dermatology and therapy, 11(1), 1–12. https://doi.org/10.1007/s13555-020-00460-1
- Knackstedt, R., Knackstedt, T., & Gatherwright, J. (2020). The role of topical probiotics in skin conditions: A systematic review of animal and human studies and implications for future therapies. Experimental dermatology, 29(1), 15–21. https://doi.org/10.1111/exd.14032
- McFarland, L. V., Evans, C. T., & Goldstein, E. J. C. (2018). Strain-Specificity and Disease-Specificity of Probiotic Efficacy: A Systematic Review and Meta-Analysis. Frontiers in medicine, 5, 124. https://doi.org/10.3389/fmed.2018.00124
- Iemoli, E., Trabattoni, D., Parisotto, S., Borgonovo, L., Toscano, M., Rizzardini, G., Clerici, M., Ricci, E., Fusi, A., De Vecchi, E., Piconi, S., & Drago, L. (2012). Probiotics reduce gut microbial translocation and improve adult atopic dermatitis. Journal of clinical gastroenterology, 46 Suppl, S33–S40. https://doi.org/10.1097/MCG.0b013e31826a8468
- Morgado-Carrasco, D., Granger, C., Trullas, C., & Piquero-Casals, J. (2021). Impact of ultraviolet radiation and exposome on rosacea: Key role of photoprotection in optimizing treatment. Journal of cosmetic dermatology, 20(11), 3415–3421. https://doi.org/10.1111/jocd.14020
- Huang, Y. X., Li, J., Zhao, Z. X., Zheng, B. L., Deng, Y. X., Shi, W., Steinhoff, M., & Xie, H. F. (2020). Effects of skin care habits on the development of rosacea: A multi-center retrospective case-control survey in Chinese population. PloS one, 15(4), e0231078. https://doi.org/10.1371/journal.pone.0231078